
Athletes engaging in big volumes of endurance exercise are at some increased risk of heart problems – in particular, arrhythmias – compared to those who do moderate exercise. The level of that risk is under debate.
At the same time, recreational athletes using heart rate monitors during their training will sometimes see numbers go up as high as 220 or 225 beats per minute (bpm). Such racing heartbeats are called tachycardia, and some of the possible underlying causes can be life-threatening.
But does a high heart rate reading on a heart rate monitor equate to this dangerous condition?
That’s what Polish doctor Robert Gajda and colleagues set out to investigate. They suspected that the super-high heart rate readings were errors, but knew that they did cause anxiety for some of the athletes in question. Even if a reading seems crazy, it can sow a seed of doubt about an athlete’s health. And that makes them important.

“I assure you, we do not get seriously sick during training and not notice it,” Gajda wrote in an email. “More than the [heart rate monitor] indications, clinical symptoms are important and should worry us … we need to inform people about the occurrence of artifacts in heart rate monitor readings, instead of sending them for senseless diagnostic procedures or abstaining from physical activity.”
They also had a second question. Regardless of whether the high readings were correct, if athletes had any other kind of heart arrhythmia, would an off-the-shelf heart rate monitor detect it and thus provide them information they could use to protect themselves?
In a paper recently accepted by the Scandinavian Journal of Medicine and Science in Sports, Gajda worked with 142 runners and cyclists who came to his Center for Sports Cardiology because they were suspected to have heart arrhythmias. All of the athletes had seen sudden, large increases in the heart rate readings on their monitors while exercising.
Under the researchers’ watchful eyes, the athletes tried to replicate these readings, this time wearing not only a heart rate monitor but also a Holter Electrocardiogram (ECG). This small device uses electrodes and provides a detailed picture of electrical signals.
“The Holter ECG is a professional device recognized worldwide by doctors as the gold standard for assessing arrhythmias in patients,” Gajda explained. “It accurately records the heart rate at a given moment of measurement, the average value of the whole record, as well as its minimum and maximum value … we see not only the heart rate but also its possible abnormalities, such as extra ventricular and supraventricular beats.”
A heart rate monitor, on the other hand, simply “detects the main electrical field produced by the heart muscle.” Instead of seeing the whole heartbeat as one would on an electrocardiogram performed at a hospital, or from a Holter ECG, a heart rate monitor simply counts what it detects as heart beats and displays that as an average rate.
“Some [heart rate monitors] with ‘beat-to-beat’ measurements and data storage capabilities do permit accurate heart rhythm analyses,” Gajda wrote. “However, these devices are also prone to artifacts that are often similar to a ‘beat’… we still do not know whether we observed the R-R distance (QRS to QRS) or only the ‘artifact peak to artifact peak’.”
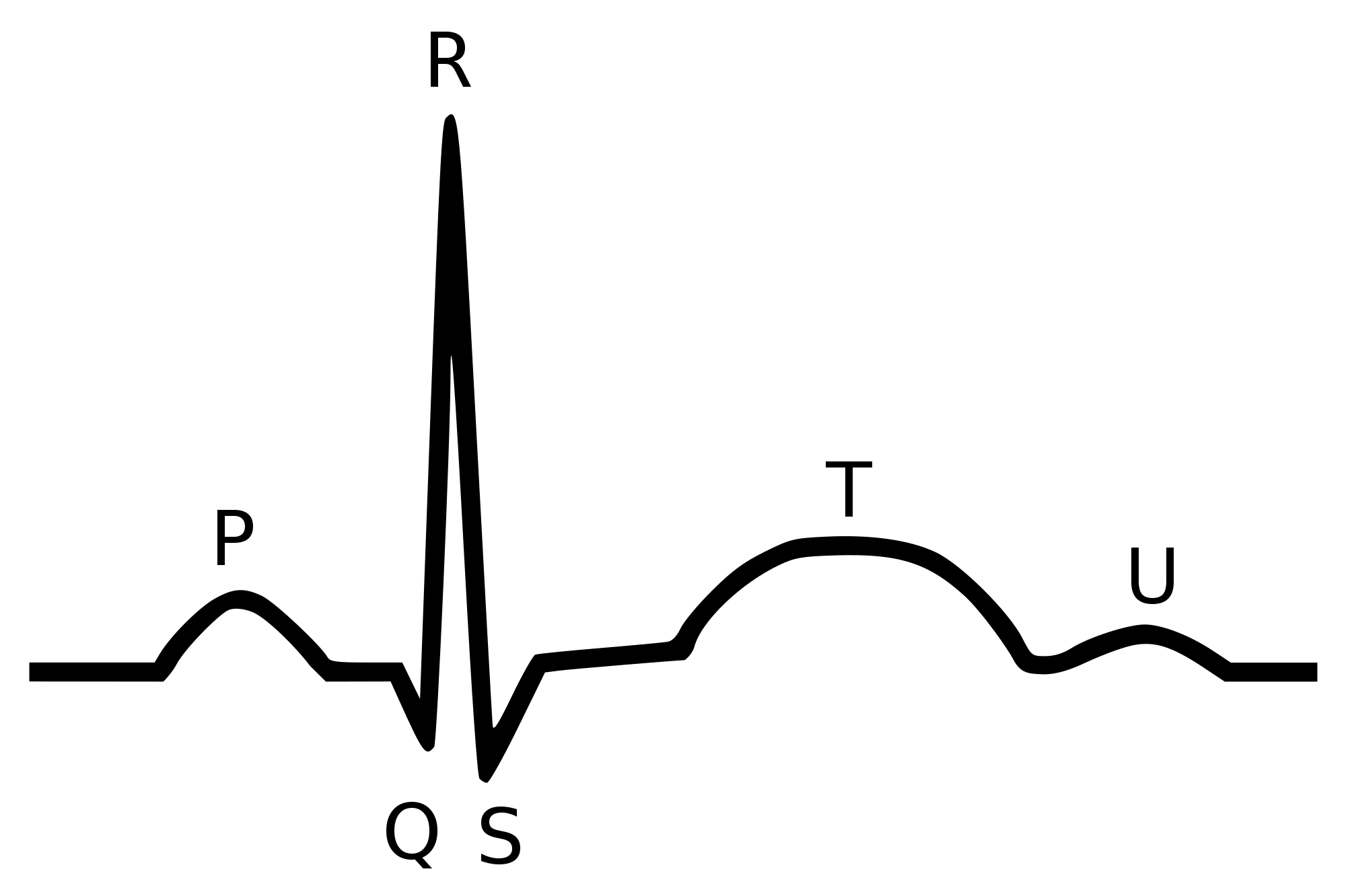
(The QRS is a phase of the heartbeat when the ventricles are depolarized before contraction, and the R wave – the middle of the QRS – is the biggest wave or peak on an electrocardiogram, as seen in the diagram at right.)
Wearing both their own normal heart rate monitors – such as the Suunto Ambit3 or a wide variety of Garmin Forerunner models – and the Holter ECG’s, the athletes were told to head out on their usual training for about an hour.
Of the group, 39 percent failed to replicate the earlier high readings. Neither their heart rate monitors nor the Holter ECG’s picked up anything abnormal, and there was also no difference between the readings provided by the two instruments in terms of average, maximum, or minimum heart rate.
A second group of athletes, about 15 percent of the total pool of subjects, picked up signs of arrhythmias on the Holter ECG but not on their heart rate monitor. These were single ventricular or supraventricular heartbeats, and, in the absence of other symptoms, don’t really indicate major heart problems.
“Every healthy person has supraventricular and ventricular beats during the Holter ECG record,” Gajda explained. “Arrhythmias have been observed in athletes with ‘healthy hearts,’ but it is not a negative prognostic factor and does not constitute grounds for abstaining from sporting activities … athletes in this group should not be concerned about these irregular beats, especially if there are no other connected clinical symptoms, for example chest pains.”
If there are those other symptoms, then it’s another story.
Most off-the-shelf heart rate monitors do not detect such single beats, because they “average out the rhythm” by counting electrical stimuli. So if an athlete has some indication that they should worry about heart disease and wears a heart rate monitor, they will not find out about these extra beats. An actual ECG would be needed.
“The value of [heart rate monitors] for detecting arrhythmias in runners and cyclists is not supported by the results of this study,” the authors wrote in the paper.
Finally, for 45 percent of athletes, an arrhythmia was indicated by the heart rate monitor: on average, a reading of 199 bpm for roughly a minute, but in the most extreme case a reading of 236 bpm for three minutes.
In only one athlete was this reading accompanied by the detection of an arrhythmia on the Holter ECG. For that athlete, it was quite clear that something serious was happening as the heart rate rose from 167 bpm to 227 bpm.
“The athlete was forced to cease training due to clinical symptoms and the sudden decrease in exercise capacity,” Gajda explained.
After resting, the rhythm went back to normal.
For the other 64 athletes, the high reading on their heart rate monitors was not accompanied by either clinical symptoms or high readings on the Holter ECG. Those athletes were not having arrhythmias. The readings were just errors.
“It is not possible to have a HR of 200-220 bpm and feel good,” Gajda wrote. “Such arrhythmia ‘cuts off’ the athlete suddenly, and even if he or she does not lose consciousness, they cannot continue to exert at the same level of intensity. Such tachyarrhythmia forces you to stop. You can’t catch your breath. You think about the worst. This is the feeling of person with severe tachyarrhythmia. You can’t miss it.”
The fact that so many athletes can encounter these faulty readings, Gajda believes, is something of a public health issue. The numbers are alarming and cause some athletes to dial back, either in that particular exercise session or in terms of how much they exercise at all.
“A physically active lifestyle is widely promoted for healthy individuals and large groups of patients,” Gajda wrote. “Millions of physically active individuals worldwide use heart rate monitors to control exercise intensity. False ‘arrhythmias’ or surprisingly high bursts of heart rate during exercise can induce fear in physically active individuals and might cause them to reduce or even abstain from training, or to seek unnecessary, time-consuming, and costly medical diagnostics. So we can say: this is a public health issue.”
The reason such anomalous readings are generated has to do with electricity. Heart rate monitors are just meant to pick up the electrical field of the heart, but many of these “artifacts” come from other electrical signals.
“Sometimes it is enough to change the position of the belt and the pulse values will return to normal,” Gajda explained. “Sometimes we run alongside the high-voltage line and the heart rate monitor goes ‘crazy’. A few meters further it returns to normal.”
A few other factors can lead to more frequent errors in the readings. For example, carrying a cellphone with you training provides additional electromagnetic waves that can disrupt transmission from the chest strap to the watch. Sometimes other athletes’ heart rate monitors create interference and errors as well.
Another source of artifacts is additional clothing either around the chest strap or the watch. For winter sports athletes, this could be a particular issue.
“There is no doubt that thicker winter clothing is conducive to the development of more artifacts,” Gajda wrote. “A thick glove on the ‘watch,’ too. Sometimes this occurs in the form of a complete disappearance of the connection between the belt and the watch … It is likely that synthetic materials that are easier to electrify may produce more distortions.”
And women, wearing sports bras, have an extra layer they have to worry about.
“The idea is for the chest strap to stick well to the body,” Gajda wrote. “This problem is beginning to be noticed by manufacturers of heart rate monitors. Today there are already some on the market that use a sports bra or shirt as the strap of a heart rate monitor (equipped with integrated electrodes). I think further development in this area will solve this problem completely.”
Then, there’s simple body movement. There are fewer artifacts in heart rate monitor data for cyclists than for runners, indicating that having a steady upper body position reduces the error rate. Gajda wasn’t sure what the cross-country skiing motion would mean in terms of these erroneous readings.
If an athlete carefully adjusts for all these factors – repositioning the chest strap, wetting the sensors so they stick to the skin better, re-arranging clothes, replacing batteries and other parts, and avoiding other sources of electrical interference – but the high readings keep coming, then they should seek out a physician even if they don’t have other symptoms, Gajda and his colleagues suggested in their paper.
But overall, his message is clear. Heart rate monitors are valuable for monitoring and controlling the intensity of training, but for detecting arrhythmias, they aren’t as great. Very high heart rate readings shouldn’t alarm athletes in the absence of any other symptoms of discomfort. The way to check whether the number is real, Gajda reminded, was to stop what you’re doing for a minute and take your pulse.
The biggest problem with anomalous readings from heart rate monitors is one of annoyance, he posits, because such artifacts make it harder to accurately track the intensity of exercise. Sure, your heart rate isn’t actually 220, which is a relief – but what is it?
“We should be upset that you do not record the training in accordance with its actual reality,” Gajda wrote. “For me, still an active runner, it is an extremely important part of the training, which informs me not only about the quality of the effort but also my form – overtraining or lack of training.”
Robert Gajda, MD, PhD, director and owner of Center for Sports Cardiology (CSC) at the Gajda-Med Medical Center in Pułtusk/Poland, is a cardiologist and sports medicine physician. His main area of research interest is physiological adaptation to endurance training as well as to extreme endurance efforts. He cooperates with Polish scientific institutes in this field. Dr Gajda is an active runner and the record holder of Polish doctors in the marathon.
Chelsea Little
Chelsea Little is FasterSkier's Editor-At-Large. A former racer at Ford Sayre, Dartmouth College and the Craftsbury Green Racing Project, she is a PhD candidate in aquatic ecology in the @Altermatt_lab at Eawag, the Swiss Federal Institute of Aquatic Science and Technology in Zurich, Switzerland. You can follow her on twitter @ChelskiLittle.



